TTS BUSINESS MEETING

In accordance with the TTS By-Laws, a Business Meeting will be held shortly after the close of the TTS 2020 Virtual Congress. The meeting will be help on Sunday, September 20, at 8 AM Montreal time and will last approximately one hour. The agenda will include an update on the TTS finances, the announcement of the TTS 2024 Congress location, a presentation for the TTS 2022 Congress in Buenos Aires, the announcement of the 2020-2022 Councilors and Officers and the official change of TTS Presidency. All members are invited to participate.
As this meeting will be virtually, we will send all members a link to join this meeting shortly before the meeting takes place.
Sincerely,
John Fung
Secretary, The Transplantation Society
SERVING THE INTERNATIONAL TRANSPLANTATION COMMUNITY

Early Bird Registration deadline soon approaching, register before July 31st.
As we wish to bring our Congress to the entire international transplantation community, and in everyone’s individual time zone, we developed a program and schedule that would allow all delegates to access the Congress programming during two time periods regardless of geographic region.
TRANSPLANTATION - HIGHLIGHTED ARTICLE

Dr. Bruce Kaplan, Executive Editor, Transplantation
Posttransplant Outcomes for cPRA-100% Recipients Under the New Kidney Allocation System
Jackson KR, Holscher C, Motter JD, et al.
Transplantation: July 2020 - Volume 104 - Issue 7 - p 1456-1461
In 2014, the United States instituted the current Kidney Transplant Allocation System (KAS). Among several changes put in place was a marked increase in priority for patients with calculated panel reactive antibodies (cPRA) of 100% (rounded up to 100%). This change has led to a substantial increase in transplants for these highly sensitized individuals. (on the order of 11 to 20 times pre-KAS numbers)
In the study by Jackson et al, the authors compared outcomes for these highly sensitized individual pre and post KAS. The study offers reassuring data that this increased rate of transplantation post KAS did not compromise short term outcomes. Unfortunately, the manuscript only could look at short term outcomes and thus does not address long term outcomes. Further the study did not assess whether these changes negatively impact non-sensitized individuals. The study by Jackson et al is a first step in what must be a broader and ongoing look at the implications of KAS.
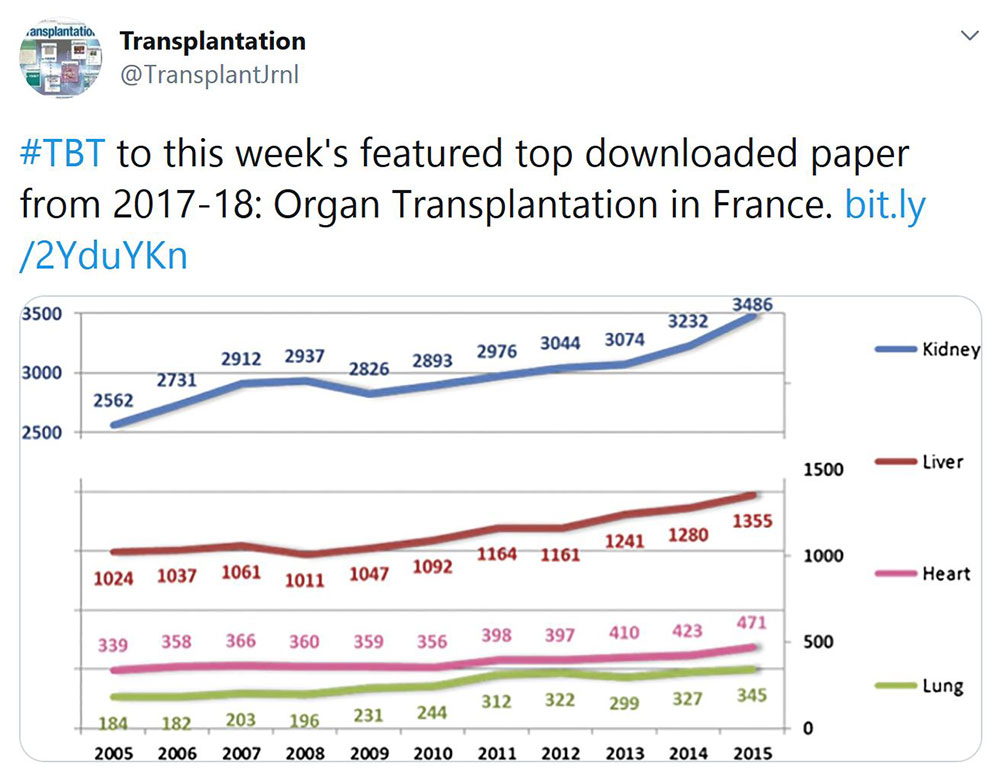
TRANSPLANTATION - WEEK'S MOST DOWNLOADED PAPER
IRTA ALLIED HEALTH PROVIDERS WEBINAR
TITLE: PEDIATRIC INTESTINAL FAILURE AND TRANSPLANT: UPDATES IN PATIENT CARE
The Allied Health Provider Committee of IRTA is pleased to present the second webinar of the Allied Health 2020 Speaker Series. This webinar will focus on patient care strategies and outcomes within intestinal rehabilitation and transplant. The topics presented will provide updates focusing on nutritional interventions, psychological challenges and psychosocial stressors in intestinal failure and intestine transplant. Each presentation will be 15 minutes in length followed by a 5-minute question period.
ISN-TTS WEBINAR: IMMUNOLOGICAL RISK ASSESSMENT AND MANAGEMENT
«HOT OFF THE PRESS» RECENT PUBLICATIONS IDENTIFIED BY TTS EDUCATION COMMITTEE ON COVID-19
This week's selection made by: Enver Akalin and Manisha Sahay

COVID-19 and Kidney Transplantation: Results From the TANGO International Transplant Consortium.
Paolo Cravedi, Sarvode Mothi Suraj, Yorg Azzi, Meredith Haverly, Samira Farouk, María José Pérez-Sáez, Maria Dolores Redondo-Pachón, Barbara Murphy, Sander Florman, Laura Goldfarb Cyrino, Monica Grafals, Sandheep Venkataraman, Xingxing Shelley Cheng, Aileen Xinqian Wang, Gianluigi Zaza, Andrea Ranghino, Lucrezia Furian, Joaquin Manrique, Umberto Maggiore, Ilaria Gandolfini, Nikhil Agrawal, Het Patel, Enver Akalin, Leonardo V Riella, TANGO study group
Am J Transplant 2020 Jul 10. doi: 10.1111/ajt.16185.
This article included 144 hospitalized adult kidney transplant recipients at 12 transplant centers in the US, Italy and Spain who tested positive for COVID-19. 65% were male with a mean age of 60 (±12) years, 40% Hispanic and 25% African-American. Prevalent comorbidities included hypertension (95%), diabetes (52%), obesity (49%), heart (28%) and lung (19%) disease. During a median follow-up period of 52 days (IQR: 16-66 days), acute kidney injury occurred in 52% cases, respiratory failure requiring intubation in 29%, and mortality was 32%. The 44 patients who died were older, had lower lymphocyte counts and eGFR, higher serum lactate dehydrogenase, procalcitonin and IL-6 levels.
Zohra S. Chaudhry, Jonathan D. Williams, Amit Vahia, Raef Fadel, Tommy Parraga Acosta, Rohini Prashar, Pritika Shrivastava, Nadeen Khoury, Julio Pinto Corrales, Celeste Williams, Shunji Nagai, Marwan Abouljoud, Milagros Samaniego‐Picota, Odaliz Abreu Lanfranco, Ramon del Busto, Mayur S. Ramesh, Anita Patel, George J. Alangade
Am J Transplant 12 July 2020; https://doi.org/10.1111/ajt.16188
This single center experience compared 35 hospitalized solid organ transplant (SOT) recipients (38 kidneys and 9 non‐kidney organs) to 100 consecutive non‐transplant controls. Chronic kidney disease (89% vs. 57% p=0.0007), diabetes (66% vs. 33% p=0.0007), and hypertension (94% vs. 72% p=0.006) were more common in the 35 hospitalized SOT recipients compared to controls. Diarrhea (54% vs. 17%, p<0.0001) was more frequent in SOT recipients. Primary composite outcome (escalation to ICU, mechanical ventilation, or in‐hospital all‐cause mortality) was comparable between SOT recipients and controls (40% vs. 48%, OR 0.72 CI [0.33‐1.58] p=0.42), despite more comorbidities in SOT recipients. Acute kidney injury (AKI) requiring renal replacement therapy occurred in 20% of SOT recipients compared to 4% of controls (OR 6 CI [1.64‐22] p=0.007). Multivariate analysis demonstrated that increasing age and clinical severity was associated with mortality. Transplant status itself was not associated with mortality.
Matthew B. Roberts, Saef Izzy, Zabreen Tahir, Ali Al Jarrah, Jay A. Fishman, Joseph El Khoury
Tranplant Inf Dis; 12 July 2020, https://doi.org/10.1111/tid.13407
This article reported 52 COVID‐19 positive SOT patients 12 Massachusetts hospitals between February 1st and May 6th, 2020. 77% were hospitalized and 35% required ICU admission. Sixty nine percent of hospitalized patients had immunosuppression reduced, 6% developed suspected rejection. Co‐infections occurred in 45% in ICU vs 5% in non‐ICU patients (p=0.037). In the first 5 days of illness, inflammatory markers were moderately increased. Subsequently, WBC, CRP, ferritin and D‐dimer increased with increasing stay in the ICU, lymphocyte counts were similar. Five patients (16%) died.
AKI and Collapsing Glomerulopathy Associated with COVID-19 and APOL1 High-Risk Genotype.
Huijuan Wu, Christopher P. Larsen, Cesar F. Hernandez-Arroyo, Muner M.B. Mohamed, Tiffany Caza, Moh’d Sharshir, Asim Chughtai, Liping Xie, Juan M. Gimenez, Tyler A. Sandow, Mark A. Lusco, Haichun Yang, Ellen Acheampong, Ivy A. Rosales, Robert B. Colvin, Agnes B. Fogo, and Juan Carlos Q. Velez
JASN June 2020, ASN.2020050558; DOI: https://doi.org/10.1681/ASN.2020050558
This case series included six black patients with COVID-19, mean age 55 years. At biopsy day, mean serum creatinine was 6.5 mg/dl and mean urine protein-creatinine ratio was 11.5 g. Kidney biopsy specimens showed collapsing glomerulopathy, extensive foot process effacement, and focal/diffuse acute tubular injury. Three patients had endothelial reticular aggregates. No evidence of viral particles or SARS-CoV-2 RNA. NanoString showed elevated chemokine gene expression and changes in expression of genes associated with acute tubular injury compared with controls. All six patients had an APOL1 high-risk genotype. Five patients needed dialysis (two of whom died); one partially recovered without dialysis.
SOCIETY OF PEDIATRIC LIVER TRANSPLANTATION:
Election for President-Elect, 2020
SPLIT are in the process of electing a new President-Elect, effective October 2020. To participate in the election you must be a Full or Allied Health Professional Member of SPLIT, with paid 2020 membership dues.
For any issues with the login, please contact Jennifer Varga, Membership Services Coordinator (membership@tts.org). For more information on SPLIT, please contact Katie Tait, Sections Manager (katie.tait@tts.org).
Click here to visit election home
We look forward to your participation in the election! Please see information on the 3 candidates below.
Evelyn Hsu |
Dr. Evelyn Hsu is a native of the midwest, born, raised and educated in Wisconsin. She completed residency in Pediatrics at the Seattle Children’s Hospital, and fellowships in Pediatric Gastroenterology Hepatology and Nutrition and Advanced/Transplant Hepatology at The Children’s Hospital of Philadelphia. She has been at Seattle Children’s Hospital since 2011, where she is currently the Medical Director of Liver Transplantation, Program Director of the Advanced/Transplant Hepatology Fellowship, and acting Division Chief. She has been an active member of the pediatric liver community, having served or currently serving in multiple leadership positions in SPLIT, AASLD, NASPGHAN, the United Network for Organ Sharing (UNOS), the American Board of Pediatrics, and the International Pediatric Transplant Association (IPTA). Her research interests and publications have centered around liver allocation to children and long-term outcomes post transplantation. |
Saeed Mohammad |
Dr. Saeed Mohammad is an Associate Professor of Pediatrics, Northwestern University Feinberg School of Medicine, and Medical Director of Hepatology and Liver Transplantation, Ann & Robert H Lurie Children's Hospital of Chicago. He has served in multiple leadership roles in NASPGHAN, AASLD, SPLIT and UNOS and currently is the director of hepatology & liver transplantation. The focus of his forty publications, and invited lectures are improving health outcomes and quality of life in chronic liver disease and transplantation. His community work includes serving with the American Liver Foundation and the Autoimmune Hepatitis Association. In addition to leading his transplant fellowship, he teaches medical and graduate school courses with a focus on decision analysis. He is proud of his mentees who are now leaders in their own right nationally. |
Shikha Sundaram |
Dr. Shikha Sundaram is an Associate Professor of Pediatrics at Children’s Hospital Colorado, where she also serves as the Medical Director of Pediatric Liver Transplantation. She has been a dedicated and active member of SPLIT since her fellowship at Lurie Children’s Hospital, including several SPLIT publications, and service as Vice Chair and then Chair of the Research Committee. She is a committed leader in Pediatric Hepatology and Liver Transplantation, chairing the Hepatology committee of NASPGHAN as well as extensive committee work for AASLD and the American Liver Foundation. She is an accomplished clinical/translational researcher, with a focus on pediatric liver disease, with more than 40 original publications to her credit. |
CORONAVIRUS (COVID-19) UPDATE DASHBOARD
The Transplantation Society (TTS) and our journal Transplantation have developed online resources to keep you informed on the Coronavirus (COVID-19) outbreak.
- TTS Coronavirus (COVID-19) Dashboard
www.tts.org/covid-19 - Transplantation Global Transplantation COVID Report
www.tts.org/txjcovid19
We are also requesting contributions and news from the transplant community to be sent to covid-19@tts.org for inclusion on our resources page.
In this dashboard, you will find links to TTS and other global and regional resources, as well as interactive maps, publications and webinars. We encourage you to explore this dashboard and share with your colleagues.
Website - www.tts.org/covid-19
Editors and contributors to Transplantation have shared their thoughts on how they are dealing with the current crisis. While we understand that the information of today may be quite different tomorrow in this fast-moving pandemic, this report will open our forum of an international exchange on COVID for the transplant community.
Website - www.tts.org/txjcovid19
Please send your own contributions and news to covid-19@tts.org for inclusion on our resources page.
IN THE NEWS
ASSESSING THE IMPACT OF DISTANCE TO KIDNEY TRANSPLANT CENTERS
July 7 - Most patients with end-stage kidney disease (ESKD) who are on dialysis will need to be referred from a dialysis facility to a kidney transplant center for a medical evaluation to potentially begin the transplant process. Currently, the United States has slightly more than 250 adult transplant centers, but there are well over 7,000 dialysis facilities throughout the country. As such, transplant centers may be less accessible to referred dialysis patients.
HOW ONE HOSPITAL CONTINUED PERFORMING ORGAN TRANSPLANTS DURING COVID-19
July 8 - For an organ transplant recipient, a virus – any virus – can be a death sentence. But for someone who needs a transplant, waiting too long to receive a new organ can be just as deadly.
WHY ARE SCIENTISTS TRYING TO MANUFACTURE ORGANS IN SPACE?
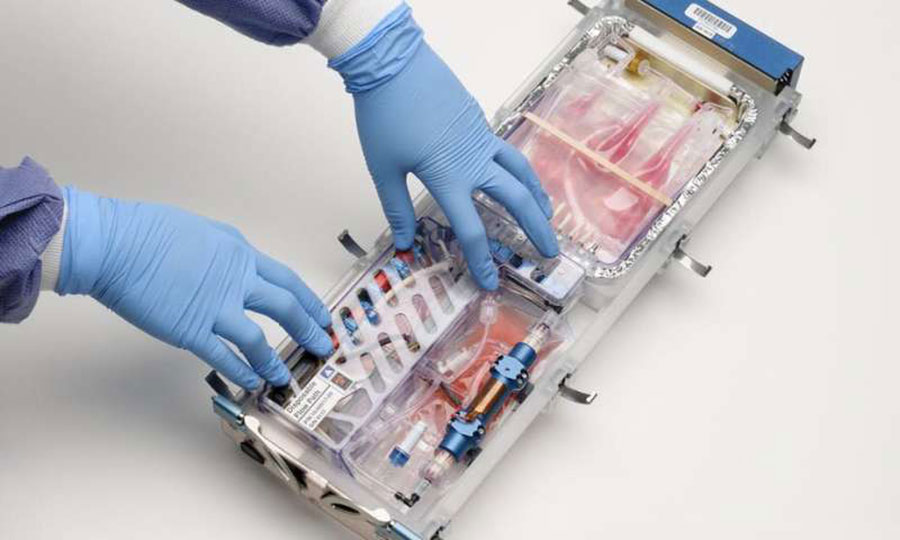
July 8 - Gravity can be a real downer when you are trying to grow organs. That's why experiments in space are so valuable. They have revealed a new perspective into biological sciences, including insights into making human tissue.
NEW STUDY WARNS OF MISINFORMATION ABOUT OPT-OUT ORGAN DONATION
July 10 - A new study has warned of the power of a type of behaviour dubbed the 'lone wolf' effect which could result in people 'opting out' of supporting organ donation. A behavioural study led by researchers from the University of Nottingham's School of Psychology and Nanyang Technological University's Department of Economics found that initial co-operation, encouraged by an opt-out policy, can be undermined by members of the public observing the actions of 'lone wolves'.
NEW HHS GUIDANCE ON SOLID ORGAN TRANSPLANTATION: REDUCING RISK AND INCREASING AVAILABILITY
July 11 - Organ procurement organizations (OPOs) and transplant centers should take note: as expected, and as outlined in our recent organ procurement and transplant alert, the U.S. Department of Health and Human Services (HHS) continues to prioritize reduction of the organ transplant waitlist by increasing access to transplantable organs.
UPCOMING MEETINGS AND ANNOUNCEMENTS
18th Asian Pacific Congress of Nephrology (APCN)
Contact
Address
The Transplantation Society
International Headquarters
740 Notre-Dame Ouest
Suite 1245
Montréal, QC, H3C 3X6
Canada
Используйте Вавада казино для игры с бонусом — активируйте промокод и начните выигрывать уже сегодня!