TTS 2020 Virtual Congress - Industry Symposiums

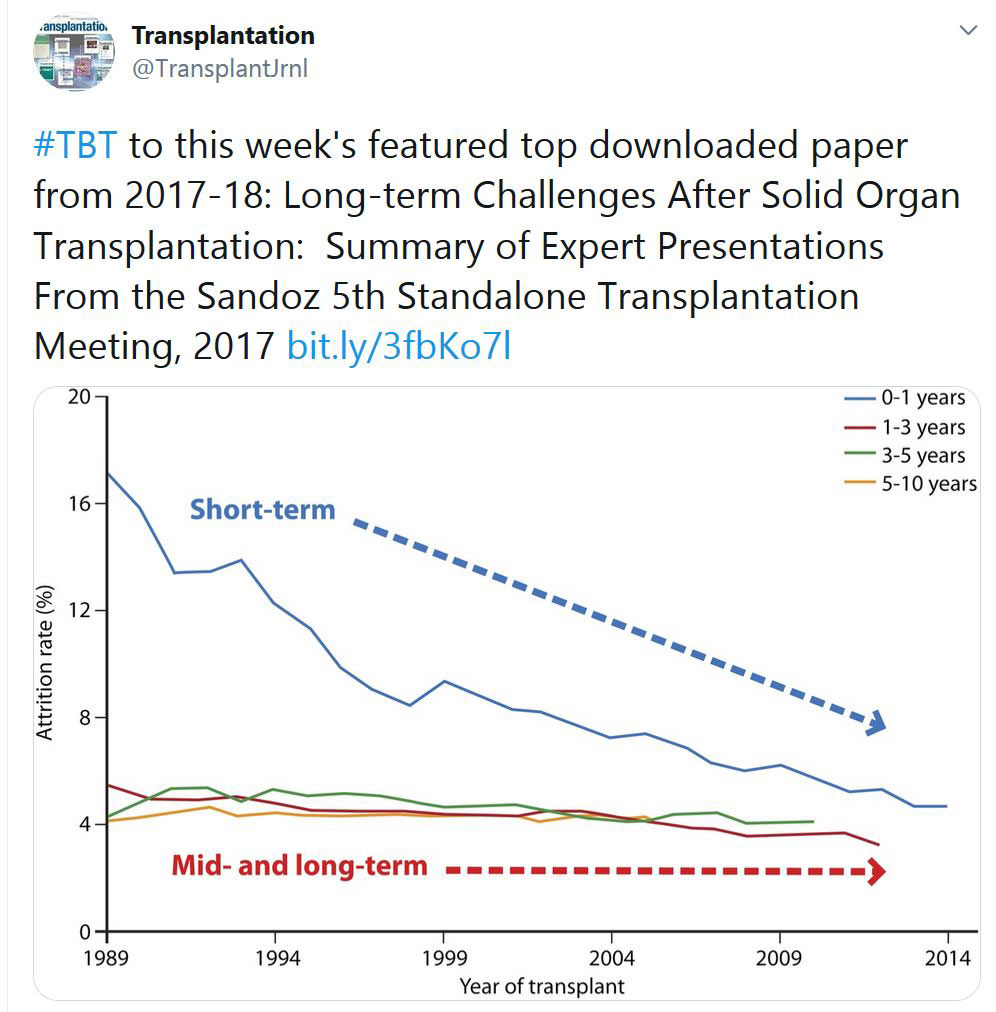
TRANSPLANTATION - HIGHLIGHTED ARTICLES
COVID-19 – in search of information? You can find a comprehensive global round up of information direct from the clinical frontline across Europe, America and Asia with information about every aspect from clinical experience to impact on clinical practice and research globally. Important information to understand no matter where you are both geographically and in terms of the level of impact of COVID-19 on your program.
«HOT OFF THE PRESS»
RECENT PUBLICATIONS IDENTIFIED BY TTS EDUCATION COMMITTEE ON COVID-19
Selected Publications by TTS Education Committee. This week's selection made by: Enver Akalin and Millie Samaniego
CORONAVIRUS (COVID-19) UPDATES
IN THE NEWS
UPCOMING MEETINGS AND ANNOUNCEMENTS
Contact
Address
The Transplantation Society
International Headquarters
740 Notre-Dame Ouest
Suite 1245
Montréal, QC, H3C 3X6
Canada
Используйте Вавада казино для игры с бонусом — активируйте промокод и начните выигрывать уже сегодня!