2022 TTS Recognition Award Winners Announced!

OUTSTANDING ACHIEVEMENT TRANSPLANTATION SCIENCE (BASIC)

OUTSTANDING ACHIEVEMENT TRANSPLANTATION SCIENCE (CLINICAL)

MENTORSHIP OR EDUCATION AND TRAINING IN TRANSPLANTATION

OUTSTANDING ACHIEVEMENT IN TRANSPLANTATION SCIENCE (DEVELOPING COUNTRY)
In Memoriam - Anthony Peter "Tony" Monaco (1932 - 2022)

Anthony P. Monaco
Anthony Monaco was a TTS Past-President, a Medawar Prize Laureate, a pioneer and a friend to all.
Beloved Husband and Father, Pioneering Transplant Surgeon and Scientist Teacher, Mentor, Collaborator, and Friend to Many, Peter Medawar, Professor of Surgery Emeritus at Harvard Medical School, and Director Emeritus of the Division of Transplantation at Beth Israel Deaconess Medical Center, died peacefully on August 22, with his family by his side.
Visit Anthony Monaco's Page on TTS.org with some articles, videos and his Medawar Prize acceptance speech.
Transplantation Updates

Transplantation - September Issue
This issue starts with a detailed examination of donor issues - including cancer transmission in Spain and several papers on perfusion to improve outcomes in heart, liver and kidney transplantation. The critical issue of artificial resumption of circulation during donation DCD is elegantly presented and discussed. Several articles present the current-day issues in Xenotransplantation - all cause for thought. COVID remains at the top of many people's agendas in transplantation, despite the waning interest in the general community, because of the important adverse outcomes in transplant recipients. There are several useful papers on COVID issues to keep us all abreast of the knowledge.
Table of Contents
Around the World
- Women Leadership in Liver Transplantation—Results of an International Survey
- Organ Transplantation in Bosnia and Herzegovina
People in Transplantation
Research Highlights
Special Article
- International Human Xenotransplantation Inventory: A 10-year Follow-up
Expert Insight
- Advancing Xenotransplantation to the Clinic: How Relevant Is the Pig-to–nonhuman Primate Kidney Transplantation Model Today?
- Expert Opinion Special Feature: Patient Selection for Initial Clinical Trials of Pig Organ Transplantation
Commentaries
- Machine Perfusion of Donor Hearts: The Next Major Advance in Cardiac Transplantation
- Ensuring the Permanent Cessation of Brain Function During Normothermic Regional Perfusion
- Donor Cancer Transmission: Focusing on the Evidence
- Four-drug Lung Transplant Immunosuppression 4EVER?
- SGLT2i After Kidney Transplantation: Ready for Prime Time?
- Commentary on “Infection Risk in the First Year After ABO-incompatible Kidney Transplantation: A Nationwide Prospective Cohort Study”
- Editorial: Optimizing Outcomes for Children Requires Ensuring Access to Living: Donor and Split Liver Transplants
Reviews
- Proceedings of the 26th Annual Virtual Congress of the International Liver Transplantation Society
- Normothermic Ex Situ Heart Perfusion With the Organ Care System for Cardiac Transplantation: A Meta-analysis
- Informed Consent for Potential Recipients of Pig Kidney Xenotransplantation in the United States
Original Basic Science
- Clamping of the Aortic Arch Vessels During Normothermic Regional Perfusion After Circulatory Death Prevents the Return of Brain Activity in a Porcine Model
- Pancreas Preservation in Modified Histidine-lactobionate Solution Is Superior to That in University of Wisconsin Solution for Porcine Islet Isolation
- A Novel High-throughput Droplet Digital PCR-based Indel Quantification Method for the Detection of Circulating Donor-derived Cell-free DNA After Kidney Transplantation
Original Clinical Science—Liver
- Varying Utilization Rates but Superior Outcomes in Liver Transplantation From Hepatitis C−positive Donors in the United States: An Analysis of the OPTN/UNOS Database
- County-level Differences in Liver-related Mortality, Waitlisting, and Liver Transplantation in the United States
- Living Donor Liver Transplant Center Volume Influences Waiting List Survival Among Children Listed for Liver Transplantation
Original Clinical Science—General
- Malignancies in Deceased Organ Donors: The Spanish Experience
- Kidney Transplantation From Deceased Donors With Vaccine-induced Immune Thrombocytopenia and Thrombosis: An Updated Analysis of the UK Experience
- Perfusate Metabolomics Content and Expression of Tubular Transporters During Human Kidney Graft Preservation by Hypothermic Machine Perfusion
- Prospective Multicenter Observational Cohort Study on Time to Death in Potential Controlled Donation After Circulatory Death Donors—Development and External Validation of Prediction Models: The DCD III Study
- Normothermic Ex Vivo Kidney Perfusion for Human Kidney Transplantation: First North American Results
- COVID-19 Infection With the Omicron SARS-CoV-2 Variant in a Cohort of Kidney and Kidney Pancreas Transplant Recipients: Clinical Features, Risk Factors, and Outcomes
- Five-year Outcome of an Early Everolimus-based Quadruple Immunosuppression in Lung Transplant Recipients: Follow-up of the 4EVERLUNG Study
- Infection Risk in the First Year After ABO-incompatible Kidney Transplantation: A Nationwide Prospective Cohort Study
- Matched Versus Mixed COVID-19 Vaccinations in Korean Solid Organ Transplant Recipients: An Observational Study
- The Efficacy and Safety of SGLT2 Inhibitor in Diabetic Kidney Transplant Recipients
Letters to the Editor
- Incidence and Severity of COVID-19 Among Vaccinated Solid Organ Transplant Recipients During the Omicron Wave
- Distinct Outcomes of Kidney Transplant Recipients With Recent COVID-19 According to the Timing of Infection
- Transplantation of Organs From SARS-CoV-2 RNA Positive Deceased Donors: The UK Experience So Far
- The Fourth Dose of CoronaVac Vaccine Results in a Small Increase of Seroconversion and Antibody Values Among Kidney Transplant Recipients
- Negative COVID-19 Plasma PCR Following COVID-19+ Donor Kidney Transplant
- Short-term Outcomes in a Nurse Coordinator–led and Nurse Practitioner–led Sotrovimab Initiative for Solid Organ Transplant Recipients During the Omicron Surge
- Perivaccination Antimetabolite Hold and Third Dose of SARS-CoV-2 Vaccine in Lung Transplant Recipients: Preliminary Report
- Informed Consent for Potential Recipients of Pig Kidney Xenotransplantation in the United States
Transplantation - Week's Most Downloaded Paper
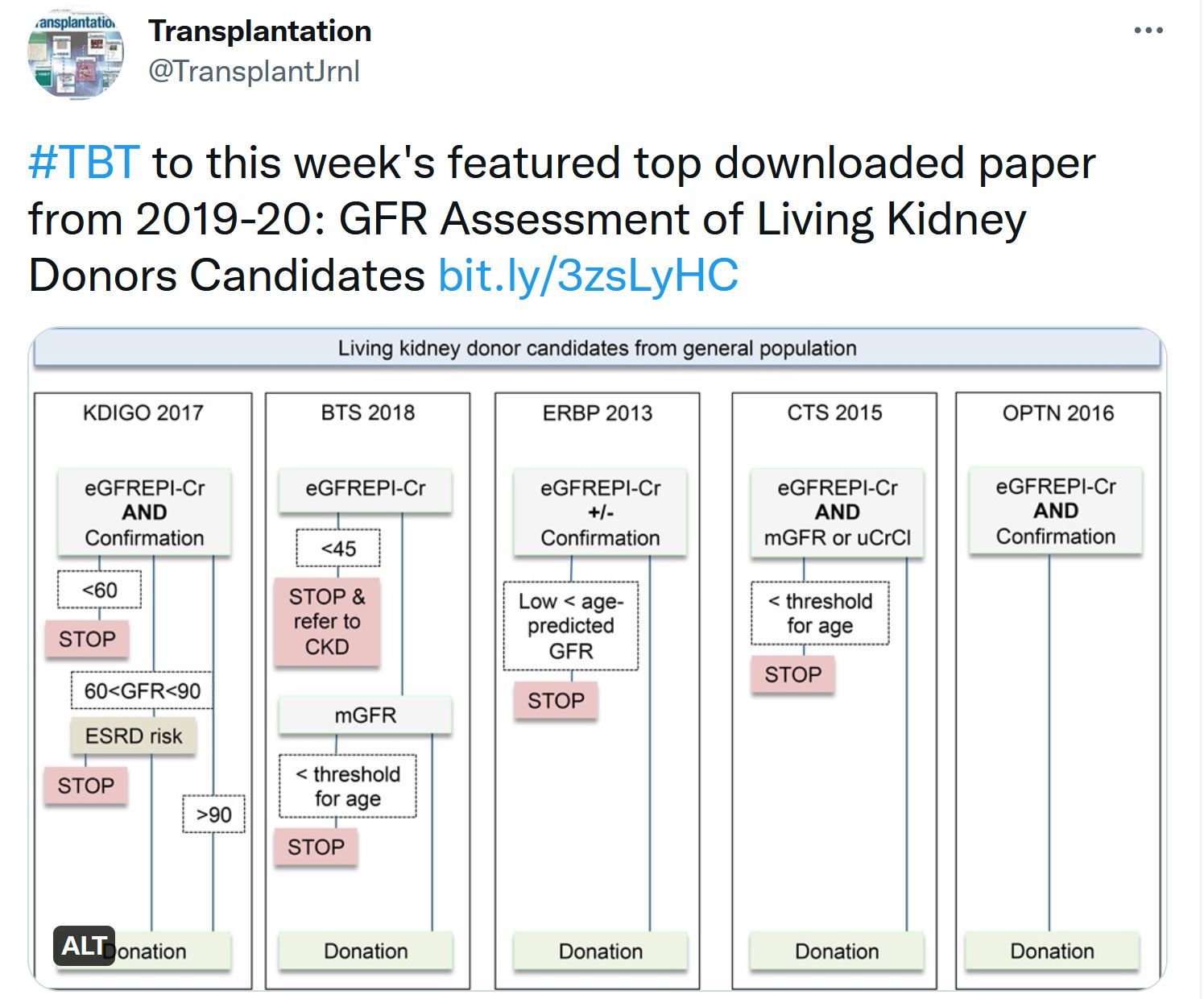
GFR Assessment of Living Kidney Donors Candidates
Living kidney donation provides the best outcomes (survival, cost, and quality of life) of all renal replacement modalities. Living kidney donors, on the other hand, are at an increased risk of end-stage kidney disease (ESKD) after donation compared with healthy nondonors for multiple reasons. Extensive pre-donation screening is required to assess eligibility for donation to avoid the rejection of suitable candidates and minimize the acceptance of donors with an increased risk of ESKD.Transplantation Direct - Highlighted Tweet
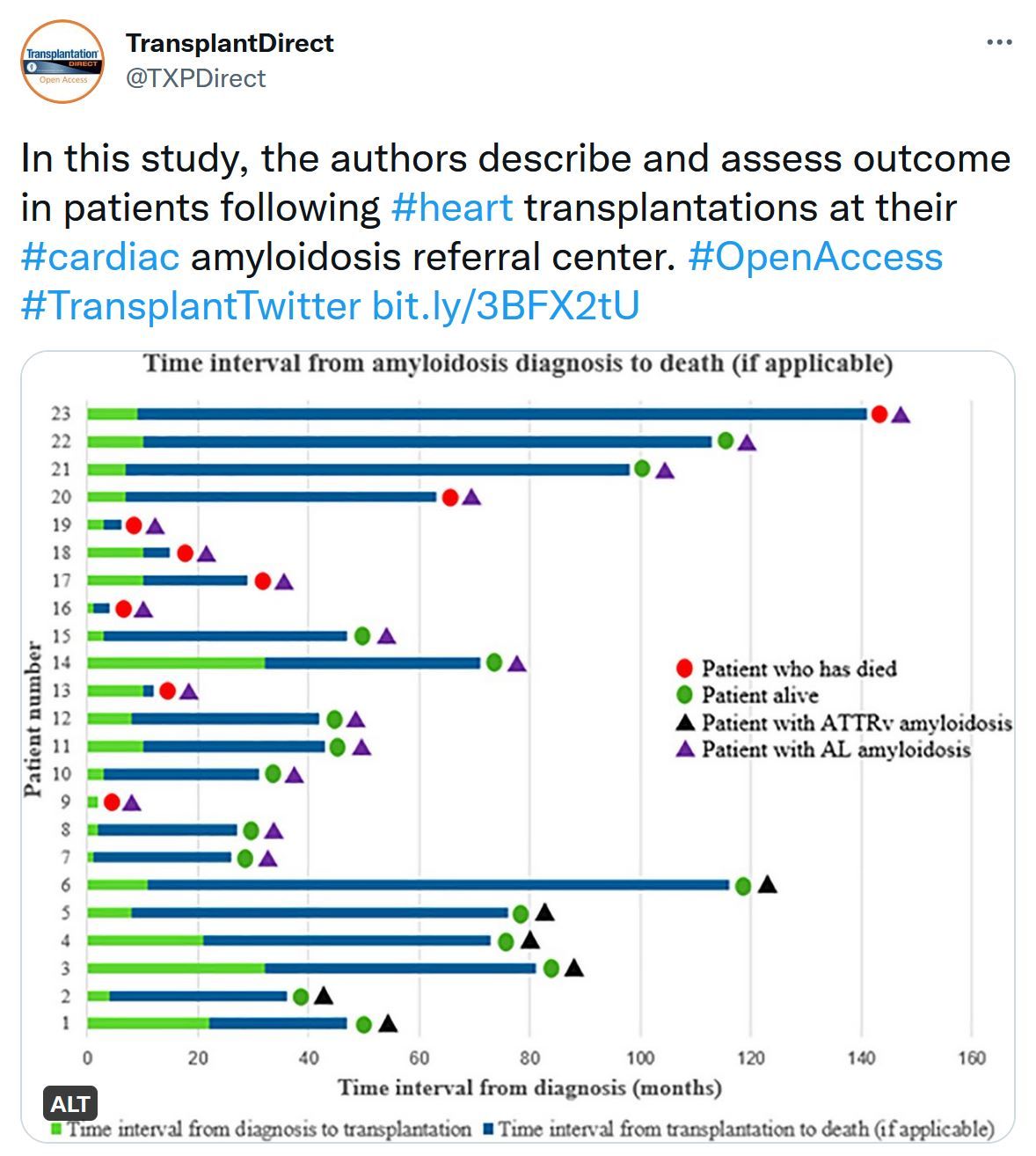
Heart Transplantation, Either Alone or Combined With Liver and Kidney, a Viable Treatment Option for Selected Patients With Severe Cardiac Amyloidosis
Heart transplantation in cardiac amyloidosis (CA) patients is possible and generally considered for transplantation if other organs are not affected. In this study, we aimed to describe and assess outcomes in patients following heart transplantations at our CA referral center.News Spotlight

Hot Off The Press
TTC Public Workshop - September 22, 2022 @ 8AM ET
TTS Needs Assessment Survey
Contact
Address
The Transplantation Society
International Headquarters
740 Notre-Dame Ouest
Suite 1245
Montréal, QC, H3C 3X6
Canada
Используйте Вавада казино для игры с бонусом — активируйте промокод и начните выигрывать уже сегодня!